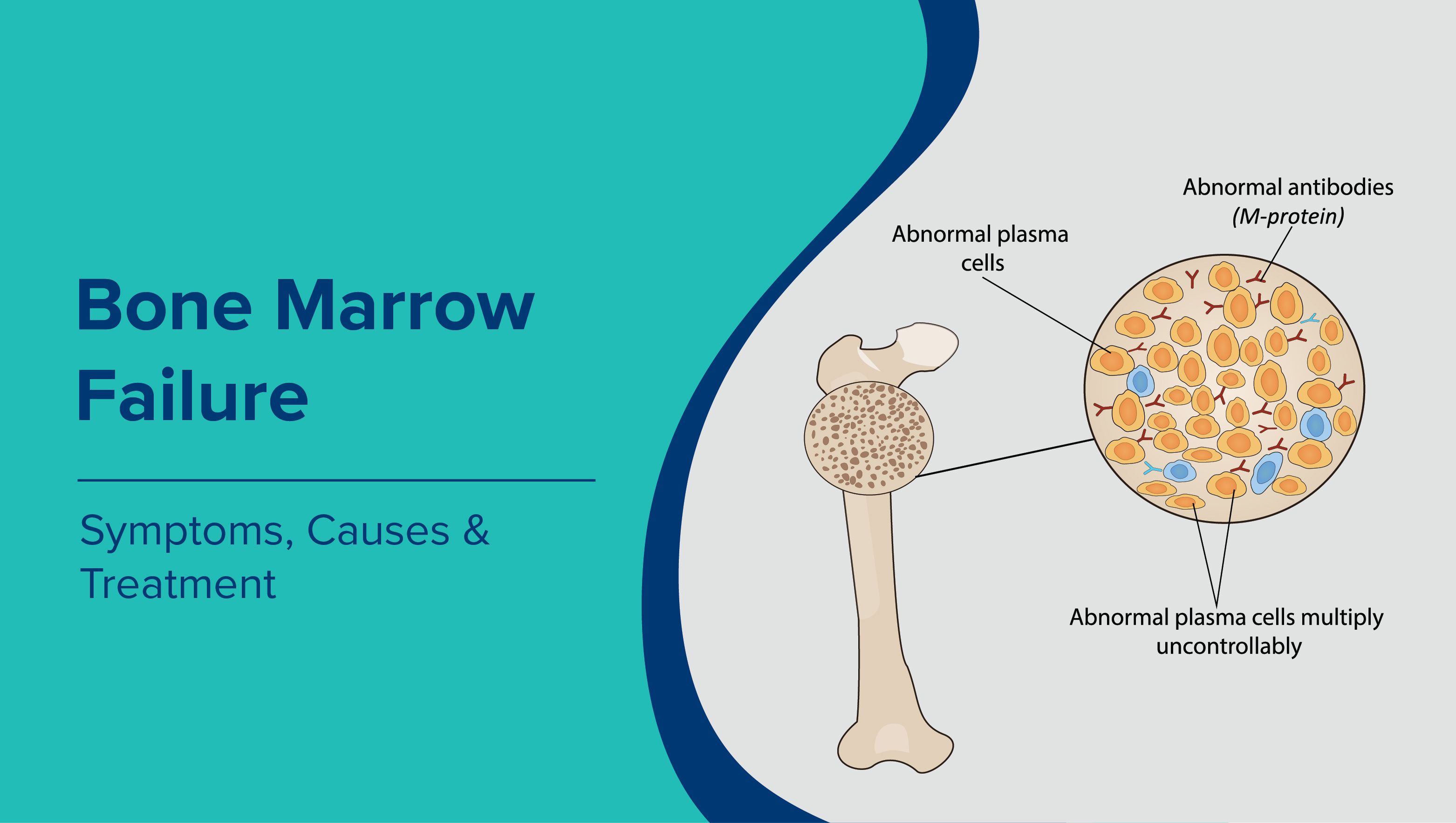
Introduction
Bone marrow failure is a serious condition in which the bone marrow cannot produce enough healthy blood cells, including red and white blood cells and platelets. This affects oxygen delivery, immunity, and blood clotting. Early diagnosis and treatment are important to prevent dangerous complications.
This guide explains bone marrow failure symptoms, causes, diagnosis, and treatment options in simple, medically accurate language.
What Is Bone Marrow Failure?
Bone marrow failure is not just one disease. It refers to a group of disorders in which the body produces fewer blood cells than normal. It can affect red blood cells (causing anemia), white blood cells (raising infection risk), and platelets (leading to bleeding problems).
Types Of Bone Marrow Failure
Aplastic Anemia: This is the most common type and can be acquired or inherited. Damage to stem cells leads to a severe drop in red blood cells, white blood cells, and platelets.Paroxysmal Nocturnal Hemoglobinuria (PNH): An acquired disorder where the immune system destroys red blood cells.
Pure Red Cell Aplasia (PRCA): This condition causes a severe reduction in the number of cells that develop into red blood cells.
Myelodysplastic Syndromes (MDS): A group of cancers where immature bone marrow cells do not develop into healthy blood cells.
Congenital Disorders: These inherited conditions, such as Fanconi anemia, Diamond-Blackfan Anemia, and Shwachman-Diamond Syndrome, affect bone marrow function from birth or early childhood.
Symptoms of Bone Marrow Failure
Bone marrow failure affects the production of all blood cell types, so symptoms can vary and affect different parts of the body. These symptoms often develop gradually, making early detection difficult.
Low Red Blood Cells (Anemia Symptoms)
If there are too few red blood cells, the body does not get enough oxygen. This can cause:
- Persistent fatigue and weakness
- Shortness of breath, even during mild activity
- Pale or yellowish skin
- Dizziness or lightheadedness
- Rapid or irregular heartbeat (book holter monitor now)
- Cold hands and feet
Symptoms of Low White Blood Cells (Leukopenia)
- Frequent or recurring infections
- Unexplained Fever
- Mouth sores or ulcers
- Slow-healing wounds
- Pneumonia or other serious respiratory infections
Symptoms of Low Platelets (Thrombocytopenia)
Platelets help the blood to clot. When there are not enough platelets, it becomes harder for the body to stop bleeding. This can lead to:
- Easy or unexplained bruising
- Prolonged bleeding from cuts or minor injuries
- Tiny red or purple spots on the skin (petechiae)
- Heavy menstrual periods
- Nosebleeds or bleeding gums
- Blood in urine or stools
If you have several of these symptoms, especially fatigue, frequent infections, or unusual bleeding, you should see a healthcare professional as soon as possible.
Causes of Bone Marrow Failure
Bone marrow failure can have many different causes, broadly categorized as acquired (developing after birth) or inherited (present from birth).
Acquired Causes
Autoimmune Disease: It is the most common cause of aplastic anemia. In this case, the immune system mistakenly attacks and destroys the blood-forming stem cells in the bone marrow. The exact cause is often unknown.Viral Infections: This can damage bone marrow directly or trigger an autoimmune response that does so. Viruses known to be associated with bone marrow failure include Epstein-Barr virus (EBV), cytomegalovirus (CMV), hepatitis viruses, HIV, and parvovirus.
Toxic chemicals: Exposure to chemicals such as benzene, which is found in some industrial solvents and pesticides, can damage bone marrow. Long-term or high exposure to these substances can reduce bone marrow function.
Radiation and chemotherapy: Patients undergoing cancer treatment may have damaged bone marrow as a side effect. Sometimes this is done on purpose before a bone marrow transplant, but it can also happen by accident.
Certain Medications: Some antibiotics, anticonvulsants, gold compounds for rheumatoid arthritis, and some anti-inflammatory drugs have rarely been linked to bone marrow failure.
Pregnancy: In rare cases, pregnancy may trigger aplastic anemia, possibly because of changes in the immune system during pregnancy.
Other Blood Disorders: Conditions such as paroxysmal nocturnal hemoglobinuria (PNH) can occur alongside or progress to aplastic anemia.
Inherited types include:
- Fanconi Anemia: A genetic disorder that disrupts DNA repair, resulting in bone marrow failure.
- Diamond-Blackfan Anemia: A condition in which the marrow cannot produce enough red blood cells.
- Shwachman-Diamond Syndrome: A rare genetic disease affecting the bone marrow, pancreas, and skeletal system.
- Severe Congenital Neutropenia: Causes dangerously low neutrophil levels, increasing the risk of infection.
- Dyskeratosis Congenita: An inherited chromosomal disorder of the telomeres that leads to bone marrow failure.
How Is Bone Marrow Failure Diagnosed?
To diagnose bone marrow failure, doctors use both clinical exams and lab tests. They usually start with a complete blood count (CBC) to check red cell, white cell, and platelet counts. Low levels of all three suggest bone marrow failure.
To confirm the diagnosis and assess its severity, doctors usually perform a bone marrow biopsy and aspiration. They take a small sample of bone marrow, usually from the hip, and look at it under a microscope. In aplastic anemia, the marrow has very few blood-forming cells.
Additional tests may include genetic testing (to identify inherited conditions), blood tests for viral infections, and flow cytometry to detect PNH clones.
Treatment Options for Bone Marrow Failure
Treatment depends on the type and severity of bone marrow failure, as well as the patient's age and health. The main goals are to restore normal blood cell production and prevent serious complications.
Bone Marrow Transplant (Stem Cell Transplant)
A hematopoietic stem cell transplant (HSCT), also known as a bone marrow transplant, is the only possible cure for severe aplastic anemia. Healthy stem cells from a matched donor, usually a sibling, are given to the patient. These cells go to the bone marrow and start making normal blood cells. This treatment is usually best for younger patients with a suitable donor.
Immunosuppressive Therapy
For patients who cannot have a transplant, often because of age or no matched donor, immunosuppressive therapy is the usual treatment. This often includes ATG to stop immune attacks on the bone marrow, cyclosporine to keep the disease in remission, and eltrombopag to help the body make more blood cells.
Blood Transfusions and Platelet Transfusions
Transfusions are a critical supportive measure used to manage symptoms while awaiting response to definitive treatment. They are not a cure but can prevent life-threatening anemia or bleeding episodes.
Growth Factors
Medications that help the body produce more blood cells, such as erythropoiesis-stimulating agents (ESAs) and granulocyte colony-stimulating factor (G-CSF), may be used to increase blood counts in some patients, especially those with MDS or milder bone marrow failure.
Antibiotics and Antifungal Medications
Patients with bone marrow failure are more likely to develop infections, so doctors often prescribe antibiotics or antifungal medications to reduce this risk. It is also important to treat any infections quickly.
Androgen Therapy
Anabolic steroids can help the body make more blood cells. They are sometimes used for people with inherited bone marrow failure or those who cannot use other treatments.
Living with Bone Marrow Failure
Managing bone marrow failure involves taking daily precautions and staying in regular contact with your doctor. Patients are often advised to:
- Avoid activities that could cause cuts or bruises when platelets are low.
- Stay away from crowded places or sick people to reduce infection risk.
- Keep vaccinations up to date as advised by their hematologist.
- Have regular checkups.
- Seek emotional support, since managing a long-term condition can be stressful.
When to See a Doctor
You should seek medical evaluation promptly if you notice any combination of the following warning signs:
- Unexplained fatigue affecting daily activities
- Frequent or unusually severe infections
- Easy or spontaneous bruising
- Prolonged or heavy bleeding
- Petechiae (small red or purple spots on the skin)
Early diagnosis greatly improves the outlook for people with bone marrow failure. The sooner it is found, the more treatment options there are and the better the chances for a good recovery.
Conclusion
Bone marrow failure is a serious condition in which the body cannot produce enough blood cells. However, new treatments like stem cell transplants and modern immunosuppressive therapies have greatly improved patient outcomes. If you notice symptoms, see a doctor quickly. Early diagnosis and treatment can make a big difference in recovery and quality of life.